Does donating blood cause iron deficiency?
Donating blood is heroic. Period.
What’s not heroic are the heavy periods that cause iron deficiency, which… don’t quite help you donate more blood.
Most blood donors are repeat donors. As a group they are single handedly keeping our blood banks afloat.
Come again?
Iron deficiency is a common problem in blood donors, with females especially affected.
A staggering 92% of blood comes from repeat donors.
That’s about 415,000 Canadians, donating over and over again for the other 40 million.
A study from Canada Blood Services revealed:
- Donor knowledge about iron is poor and few donors discuss blood donation with their physician.
- Repeat donors are often iron deficient (i.e., low ferritin) despite passing a hemoglobin screen.
- Most donors failing their hemoglobin screen are iron deficient.
- Donors with low ferritin are not always advised to take iron supplements by their physician.
- Many donors will start iron supplementation if advised to do so by their physician.
Protecting our heroes
To help guard against this, female donors are limited to being allowed to donate every 84 days. That’s because it takes at least that long to recover from the 500 ml blood (250 mg of iron, 250 hamburgers) donated.
As another layer of protection, hemoglobin is measured on-the-spot at donation centres, but as you know, anemia and iron deficiency are not the same thing. Instead, doctors and patients alike could be more on-the-ball with keeping an eye on ferritin, and bumping it up >100 μg/L whenever it gets low.
Since January 2023, Canadian Blood Services has also been selectively testing female donor blood for ferritin, by their 10th donation. Those with ferritin <25 µg/L are notified, and advised to wait six months before donating whole blood again. Better than nothing, but a little late.
One slow pill at a time
If attacking the deficit orally, 8+ weeks of 40 mg of iron supplementation is supposed to recover the lost iron from one donation.
That’s only if there’s no other risks present that make it challenging to absorb the iron or lose the iron (i.e., menses, vegetarianism, gut problems…).
Then, the only way to know if oral iron is even working for you is to re-test. You already know the importance of ferritin, but if you’re anemic, you can also do this by seeing if your hemoglobin has gone up by at least 10 mmol/L in 2 weeks.
If it hasn’t, ask your doctor for, or reach out to us, to get an IV.
Dear doctor
So how can we, as doctors, do our part to protect our donor heroes?
We should be checking ferritin in males who donate 3 times per year and females who donate once per year.
We should emphasize that anemia is not the threshold to decide if someone should or shouldn’t give blood. Iron deficiency without anemia is an equally valid threshold.
We should make sure the iron supplementation you’re taking is working for you (by raising your ferritin closer and closer to 100). We shouldn’t assume it is.
We should offer repeat donors iron infusions to replenish their stores quickly and effectively so they can continue to donate if they so desire and improve their overall wellbeing.
And that's all we've got
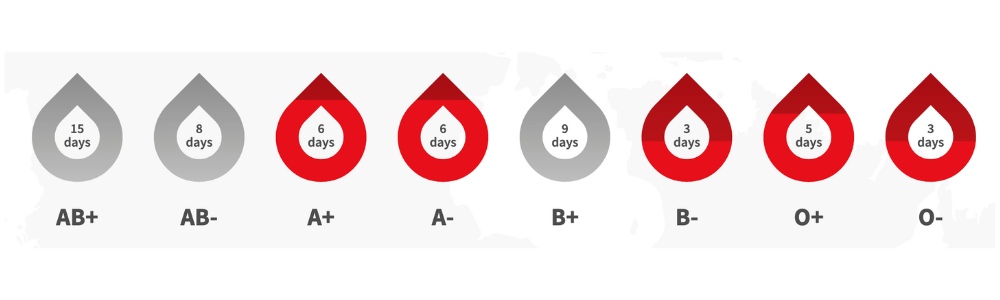
Or, hear it from...
“if you don’t have enough iron, how in the hell you gonna donate your blood to somebody else?”











